Hunter Seven Foundation Shines Light on the Impact of Environmental Toxic Exposures to Veterans
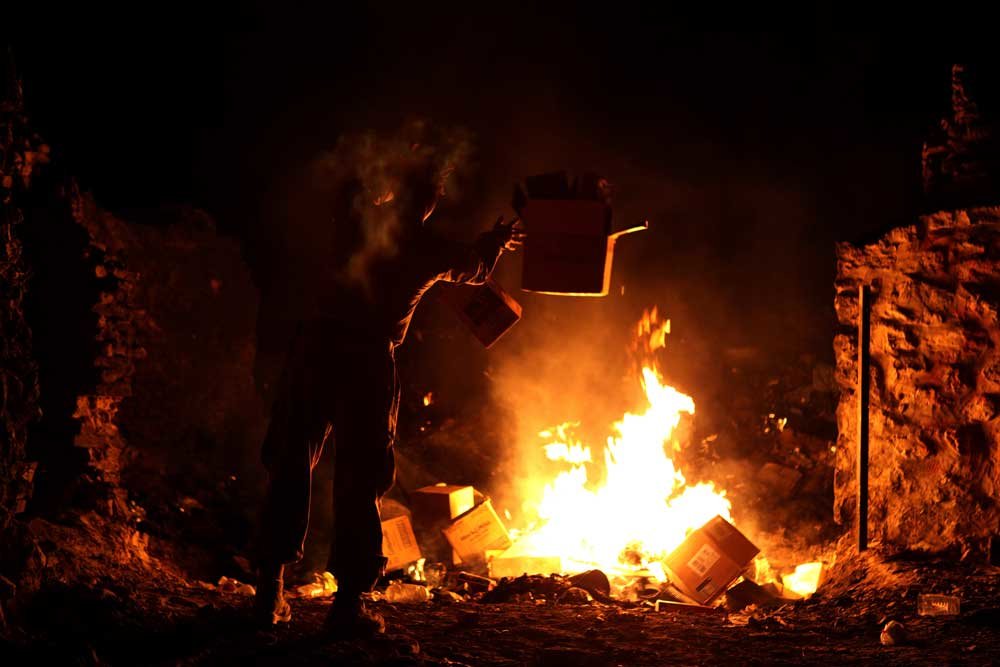
US Marine Lance Cpl. Richard Carmichael with the Warfighter Exchange Service Team, Combat Logistics Regiment 2, disposes of trash at the burn pit in Forward Operating Base Zeebrudge, Helmand province, Afghanistan, in 2013. US Marine Corps photo by Sgt. Anthony L. Ortiz.
Sgt. Maj. Robert Bowman, an Army Ranger assigned to a Recon platoon, deployed to Mosul, Iraq, in 2004 for 12 months as part of Operation Iraqi Freedom (OIF), operating under the call sign “HUNTER-7.” Bowman returned to Iraq for another 15 months in 2007 to support the surge — this time in and around Baghdad. Bowman was liked and well respected by his fellow soldiers.
“Every time I heard Bowman’s voice come over the radio,” one of them said, “I felt safe. He had a calming nature to him that always assured me in times of heated battles, that it would be okay.” His wife, Colleen, said Rob was a true “guy’s guy,” who taught each of their four daughters how to shoot and bait their own fishing hooks.
Upon returning from his second deployment, Bowman began to experience unexplained flulike symptoms. He failed a physical for his next assignment and, soon after, was diagnosed with cholangiocarcinoma — an extremely rare form of bile duct cancer. Bowman succumbed to his illness and passed away on Jan. 13, 2013. He was just 44 years old.

Former Army medic Chelsey Poisson heard about Bowman from her boyfriend (now fiance) Kyle Simoni, who had served with Bowman in Iraq. Poisson also learned Bowman was one of five soldiers in his platoon who died after returning home. Furthermore, she discovered at least 15 others from the same platoon still suffer from a wide-ranging rash of symptoms, including sleep apnea, Crohn’s disease, tumors, vitamin D deficiencies, and endocrine problems.
These disturbing findings inspired in Poisson and Simoni the idea to organize a group of volunteer veterans to raise awareness, and provide solutions, for veterans impacted by toxic exposures. Their brainchild became known as the Hunter Seven Foundation, honoring the late Bowman. Headquartered in Providence, Rhode Island, H7F launched in June 2018 and was officially registered as a 501(c)(3) nonprofit shortly thereafter.
The formation of H7F could not have been better timed. During this period, Poisson was finishing an undergraduate nursing degree at Rhode Island College, honing her interest in research. She was learning how to recognize anomalous data, and the patterns of illness among her fellow veterans did not sit well. Fortunately, her connection to RIC gave Poisson the opportunity to channel her concerns into an independent honors course and leverage the academic resources at the college to facilitate a formal study, normally an activity reserved for doctoral and graduate-level students. Two professors of nursing at RIC lent their support — Lt. Col. Sheri Boucher (a 29-year Air Force veteran) and Dr. Sylvia Ross. As a testament to the validity of Poisson’s research, her study recently appeared in the 2020 International Journal of Environmental Research and Public Health, the first of its kind to be published worldwide.

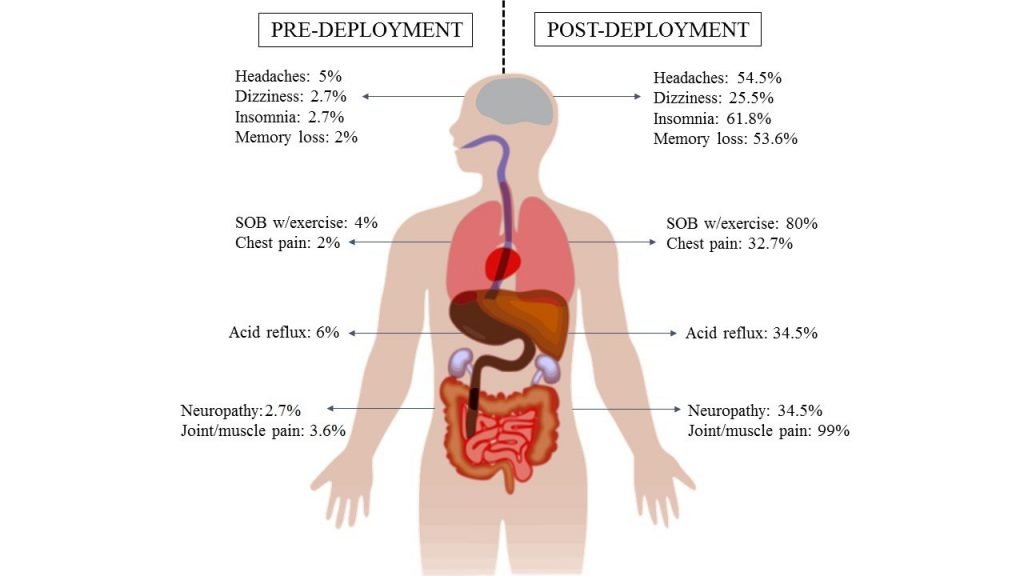
Her findings revolved around a survey of 110 veterans from the war in Iraq who “reported a decrease in overall physical fitness and increased respiratory clinical symptoms compared to pre-deployment periods.” Furthermore, the survey revealed a common thread connecting these respondents: Nearly 90 percent of them reported frequent exposure to smoke and fumes from open burn pits.
Burn pits were a common means of waste disposal at US military base camps in Iraq and Afghanistan between 2000 and 2018. Backhoes were used to dig these large, open pits in the desert, which became dumpsites for nearly everything, including plastic bottles, tires, food scraps, various solvents, and unfired ammunition. Trash was typically ignited with jet fuel and gasoline. Once lit, the fires could burn continuously, around the clock. Poisson read some accounts that alleged pharmaceuticals, medical waste, animal carcasses, and even human remains were incinerated in some pits.
According to the Hunter Seven Foundation, by May 2003, American forces in Iraq had constructed and operated more than 250 burn pits on Joint Base Balad alone. One Air Force official who conducted an official assessment of Balad in 2006 concluded it was the “worst environmental site” he had personally visited. The report went on to warn that the smoke being generated posed potentially “chronic health hazard” to individuals. Reliable estimates suggest every soldier in a combat zone creates approximately 10 pounds of trash per day. Assuming that number is accurate, the 36,000 service members and contractors who occupied Joint Base Balad during a given month generated approximately 360,000 pounds of waste during that period — more than 4 million pounds per year.
The Hunter Seven Foundation is not only armed with the knowledge required to bring awareness to the hazards and consequences of toxic environmental exposures to our veterans, it is uniquely qualified to help those who have been impacted as well. “We’re the only group in the world that does what we do,” said Poisson. “We’re the only veteran-founded organization that volunteers to do this [type of work]. We’re also the only organization that has a complete medical staff. Everyone on our team has some sort of advanced medical degree and license to practice medicine. We bring a unique set of skills to the table.”
Since publishing her study, Poisson has graduated and begun practicing both as a trauma nurse and clinical researcher in the field of infectious diseases. She now holds master’s degrees in nursing and public health as well. Her colleagues at H7F include an equally impressive list of credentialed health care professionals, including research nurses, medical students, and doctors.
H7F interacts with many organizations regarding veteran health. However, Poisson has found that the vast majority of them are more focused on receiving disability compensation than practicing health care. “I get it,” she said. “I’m a disabled veteran myself. I was medically discharged with a severe spinal cord injury so, yeah, I get it. But money is not going to save your life. […] We are an all-volunteer organization that just focuses on health care.”
“I’m a disabled veteran myself. I was medically discharged with a severe spinal cord injury so, yeah, I get it. But money is not going to save your life. […] We are an all-volunteer organization that just focuses on health care.”
She went on to explain there are three tiers of health care: primary or preventative care measures, or essentially, don’t get exposed in the first place; secondary prevention, which aims at screening and early identification to rapidly seize any health concern from worsening; and tertiary care, which focuses on treating chronic conditions and managing end-of-life issues. H7F focuses on the secondary tier, and realizes the importance of screening patients so problems can be nipped in the bud before they become debilitating or life-threatening.
“As a veteran myself,” continued Poisson, “I can recognize veterans by the slogan on their T-shirts or the tattoos they wear. But the majority of health care workers can’t do that. To make matters worse, only 25 to 27 percent of Iraq-Afghanistan veterans utilize the VA, so we’re missing nearly three-quarters of the men and women who are coming home who are potentially exposed. In recent memory, I’ve lost two veterans in the past two weeks. Both were misdiagnosed for over two years. In each case, their symptoms were brushed off as psychosomatic issues or normal aging. At H7F, we try not to blame the VA, DOD, or members of Congress because this is a health care problem. We need to work together to help save, prolong these veterans’ lives.”
H7F has used the data gathered in its research projects to develop a software application that has become instrumental in helping providers screening veterans for potential exposure issues. Therefore, providers who would not be otherwise equipped to recognize pattern symptoms unique to veterans who served in Iraq, Afghanistan, and other countries in the Global War on Terror now have a resource to guide them through a systematic, evidence-based diagnostic process.

When asked about any noticeable trends in her research, Poisson shared that preliminary data suggests chronic symptoms of toxic exposure seem to be much less prevalent among Afghanistan veterans than those who served in Iraq. “One of the things we chalk that up to is Iraq is an arid region. On average, temperatures can range from 90 to 130 degrees and it’s a very dusty place. The only way to exercise over there is to run. You run outside on the base and it’s really hot out. Physiologically speaking, your work and breathing increases. You’re sweating more. Your lungs are working harder and your blood capillaries are really opened up. So you’re actually breathing in more particulate matter and taking them deeper into your lungs. And who knows what’s in that sand?”
A recently retired Navy nurse and member of the H7F medical team, Lt. Cmdr. Nikki Selby knew there was a problem after working in the military’s oncology department: “I kept seeing these younger, otherwise healthy men and women on the floors, being treated for rare cancers, sarcomas, and it just didn’t make sense.” Selby pointed to the lack of screening as a big problem. “We know the rate of colon cancer is growing in young veterans,” she said. “But when you ask to be screened, they refuse because you are too young, or don’t fit the profile […] yet this is one of the biggest causes of cancer-related deaths in the post-9/11 veteran population.”
Burn pits are only the tip of the spear. H7F data also shows tuberculosis as another common source of exposure. We don’t normally screen for TB in North America because the disease has largely been eradicated here. “But when you’re a military police officer working at a high-risk prison like Abu Ghraib,” observed Poisson, “TB is a real possibility. And it’s often overlooked.”
The Hunter Seven Foundation has made great strides in a short period of time but there is still much work to be done. Poisson has a great deal of confidence in her colleagues. “Our team is thoroughly screened and deeply rooted in honesty and service. Each individual has a specific experience and specialty in either medicine or research and military service. We serve on a 100% voluntary basis and do this for the love of each other.”
If you are a veteran struggling with undiagnosed issues, or know one who is, visit hunterseven.org. You can also reach H7F via Facebook and Instagram (@HunterSevenFoundation).

Tim Cooper is a contributing writer for Coffee or Die and has been a freelance writer for more than 20 years. He is also a certified firearms instructor and soon-to-be-famous recording artist with Fat Chance Records. When Tim is not traveling the world on assignment, which is actually more often than not, you will probably find him at a nearby shooting range or sitting behind a drum kit, staring at his bandmates in bewilderment.
BRCC and Bad Moon Print Press team up for an exclusive, limited-edition T-shirt design!
BRCC partners with Team Room Design for an exclusive T-shirt release!
Thirty Seconds Out has partnered with BRCC for an exclusive shirt design invoking the God of Winter.
Lucas O'Hara of Grizzly Forge has teamed up with BRCC for a badass, exclusive Shirt Club T-shirt design featuring his most popular knife and tiomahawk.
Coffee or Die sits down with one of the graphic designers behind Black Rifle Coffee's signature look and vibe.
Biden will award the Medal of Honor to a Vietnam War Army helicopter pilot who risked his life to save a reconnaissance team from almost certain death.
Ever wonder how much Jack Mandaville would f*ck sh*t up if he went back in time? The American Revolution didn't even see him coming.
A nearly 200-year-old West Point time capsule that at first appeared to yield little more than dust contains hidden treasure, the US Military Academy said.












