
For those training to be Special Forces medical sergeants, a year of academics, field training, and practice in a classroom leads to a monthlong rotation at a real hospital. Coffee or Die Magazine shadowed a class through their time at two busy ambulance and emergency room rotations in Camden and Trenton, New Jersey.
How the Special Operations Combat Medic Course Provides Real-World Training
The car was white with no lights on, and something looked off.
Maybe it was parked too far from the curb. Perhaps it was the alley where it was parked, a run of cracked asphalt that ended in a rubble of broken concrete and weeds, deep inside a Camden, New Jersey, neighborhood.
As the ambulance slowed next to the sedan, two civilian paramedics and a US Army medic inside peered at it. The 911 call had come a little after 10 p.m., but the street was deserted.
They jumped out of the ambulance and saw a man behind the wheel, dead or passed out. Did he come here to shoot up in a quiet place? Or was he driven there by someone who didn’t want him found too quickly?

Daniel, a Special Forces medic trainee, works a patient that he and his ambulance team found passed out in a car on a dark street. Daniel sat in the cars backseat to reach forward to the man, squeezing a football-shaped bag to breath for the man. Photo by Matt White/Coffee or Die Magazine.
They opened the car’s doors. He still didn’t move. They laid his seat back. Motionless.
Daniel was a year into his training to become a Special Forces medical sergeant, and now his eyes spotted the drug paraphernalia. It was an overdose.
He prepped a vial of Narcan, a drug that reverses the effects of opioids so overdose patients can breathe again, and injected it into a vein running up the man’s upper arm. Almost immediately, the driver began to stir.
This was the most dangerous minute, what medics call “wake-up,” when the patient revived by Narcan turns belligerent, even violent, because someone killed the high.

Medics from across US special operations forces train at SOCM to ensure that medics in every branch have the same level of training and can work together in the field. Photo by Matt White/Coffee or Die Magazine.
But that didn’t happen on this call, probably because even though he awoke, this man was in bad shape. Daniel hopped in the back seat and held an oxygen mask over the driver’s mouth, pumping a football-sized rubber ball to help him breathe. Minutes later, the medics had the man on a stretcher, then into the ambulance, and off to Cooper University Hospital, home base for all the military medics in Camden.
It was a simple medical call, one of over a dozen Daniel would respond to in his shift. But he got to practice finding weak vital signs, “pushing meds” to a sick patient, and figuring out a medical puzzle to save a life. It was a lot easier than Daniel’s first call in Camden. A car hit a woman, and she needed to have her shattered pelvis stabilized. The second call was a kid hit by a car. But he wasn’t just any child, but part of a local street crew that drives through the city on dirt bikes and four-wheelers.
“They thought we were gonna take him to jail,” Daniel said. “The guys on dirt bikes were pounding on the door of the ambulance. Pretty great experience.”

A student in the Special Operations Combat Medic Course boards an ambulance while working alongside emergency medical technicians from Cooper Trauma Center in Camden, New Jersey. US Army photo by K. Kassens.
That call ended with the kid trying to bite the Green Beret-in-training.
So compared with most nights in Camden, an overdose in a car on a deserted street is easy. On paper, it was a few boxes checked on a training sheet, but those who know urban medicine would recall it as a few moments in a long shift during the toughest medical course in the military.
*****
Originally created to train Special Forces medics on a mix of dirt medicine and high-tech equipment, the Army’s Special Operations Combat Medic Course, known as SOCM, is now where virtually every frontline medic in US special operations is trained.
In any given class, sailors headed to Naval Special Warfare units and soldiers assigned to Army Ranger battalions train alongside corpsmen destined for Marine Raiders or Recon units and future 18-Deltas bound for Special Forces. Besides direct action ground medics, SOCM also trains flight medics who want to join the 160th Special Operations Aviation Regiment and others going to Army Civil Affairs units who might one day work side by side with Special Forces units (one notable missing special ops component is Air Force Pararescue, which has its own medical pipeline).
Endless rounds of pushups and long ruck marches are the key to most special ops training, but not SOCM, where students rise or fall on academics and medical knowledge. Still, the attrition rate here is higher than at Ranger School.
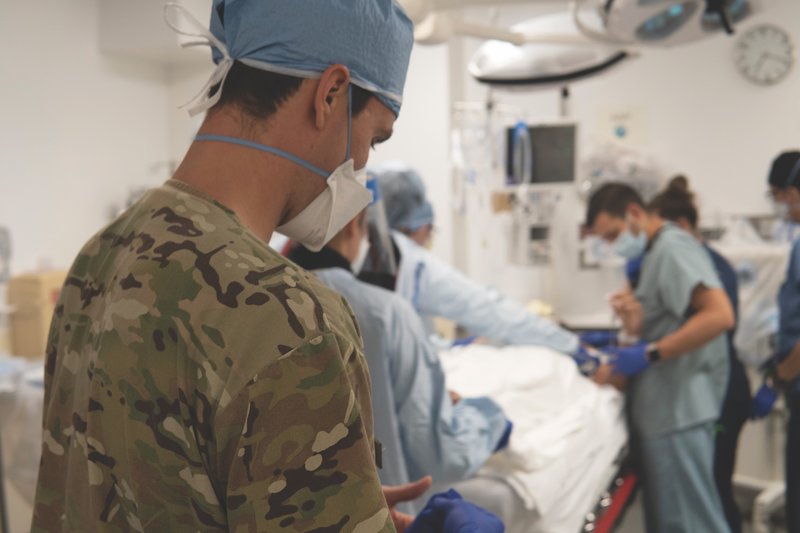
A SOCM student during treatment and assessment of a patient at the emergency department at Cooper University Hospital in Camden, New Jersey. SOCM students wear camoflague scrubs at the hospital to distinguish themselves from other students at Cooper, a full-time teaching hospital. Photo by Matt White/Coffee or Die Magazine.
Before students ship out to places like Camden for clinical rotations, they spend close to a year at Fort Bragg, North Carolina. The first cut comes from academics, a fire hose of basic anatomy and physiology and clinical instruction. Those who survive move on to trauma care, which culminates in students completing stressful and timed exercises that force them to quickly diagnose, treat, and package a simulated patient or patients with multiple injuries.
By this point, a starting class of 100 candidates might be down to 40. Those survivors enter the clinical rotations in New Jersey, Tampa, Florida and a handful of other major cities nationwide. They’ll spend a month working 24-hour shifts on ambulances and in emergency rooms.
Those assigned to New Jersey rotate between Camden and Trenton, about an hour away.
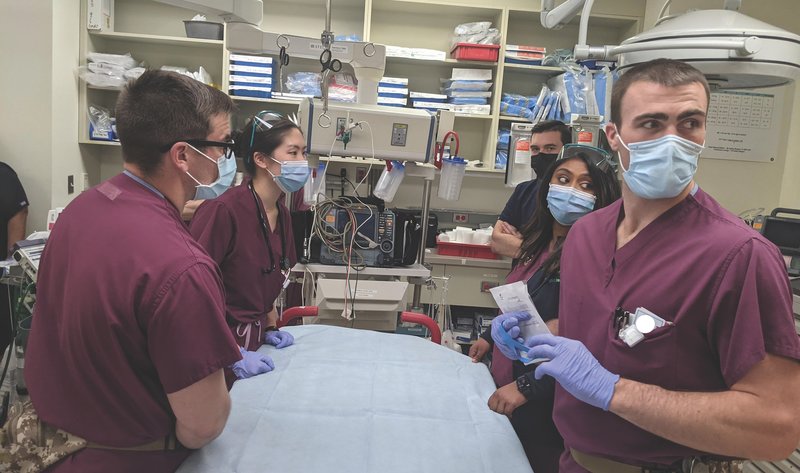
Two SOCM students, front left and front right, await an incoming trauma patient in the Emergency room at Capital Health Regional Medical Center in Trenton, NJ with the hospitals ER staff. The student on the left is training to be a flight medic with the 160th Special Operations Aviation Regiment while the student on the right quit a job as a college football coach to be a Special Forces medic. Photo by Matt White/Coffee or Die Magazine.
Those two New Jersey river cities — each former manufacturing hubs that lost jobs and industries in recent decades — are two of the most violent in America. FBI crime stats estimate that 16 out of every 1,000 Camden residents became victims to violent crime in 2020, four times the national average. In Trenton, it’s 11 out of every 1,000.
During a typical rotation, a military trainee likely will perform critical trauma procedures that a medic in a regular combat unit might not encounter during an entire career
— placing chest tubes and needle decompressions, intubating patients, reducing fractures, administering advanced cardiac drugs and painkillers, maybe even performing pericardiocentesis, when a long needle is inserted into the heart to drain excess fluid.
In both Camden and Trenton, students are overseen by trauma surgeons with combat experience as US Army Reserve doctors.

Dr. John Chovanes at Camp Bastion surgical hospital during the Third Battle of Fallujah in 2016. Photo courtesy of John Chovanes.
At Camden’s Cooper University, Col. John Chovanes oversees the hospital and emergency medical services rotations. As a junior surgeon on Sept. 11, 2001, Chovanes drove alone to Manhattan to join rescue crews working at ground zero.
He ended up treating two trapped Port Authority Police officers for hours while rescuers freed them. The two were the last survivors pulled alive from the World Trade Center’s wreckage.
Later as an Army surgeon, he deployed on forward surgical teams with Special Forces, often receiving critical patients handed off from 18-Deltas in the field.
In Trenton, Lt. Col. Michael Kelly oversees the course for
the special ops medics at Capital Health Regional Medical Center. Also an Army Reserve surgeon, Kelly deployed to work in the heart of Special Forces operations in Afghanistan’s Kandahar province in 2016.
“It was fairly kinetic and I worked a lot with the 18-Deltas on the team,” Kelly said. “I thought they were amazing, really bright guys. They were always eager to learn. Whenever we had downtime, we were always talking about things.”

Dr. Michael Kelly, an Army reserve surgeon, oversees SOCM training at Capital Health Regional Medical Center. Photo from Capital Health Facebook.
On days with more patients than doctors, Green Beret medics would scrub up and join Kelly in surgery, offering an extra set of trained hands, sometimes performing complicated trauma procedures under the doctor’s guidance.
“When I got back from that deployment. I knew that Dr. Chovanes had started — or was in the process of starting — the [SOCM] program of training those guys here,” he said.
The two docs have been connected long before they were Army surgeons. As an 18-year-old in New Jersey, Kelly became a father. He suddenly needed a job that provided health insurance and that would let him attend college at Rutgers University-Camden during the day. He answered an ad for an overnight medical clerk position at Cooper and ended up in the emergency department, where he met a new surgeon, Chovanes.
“He saw me sitting at the nursing station desks in there and studying biology,” he said.
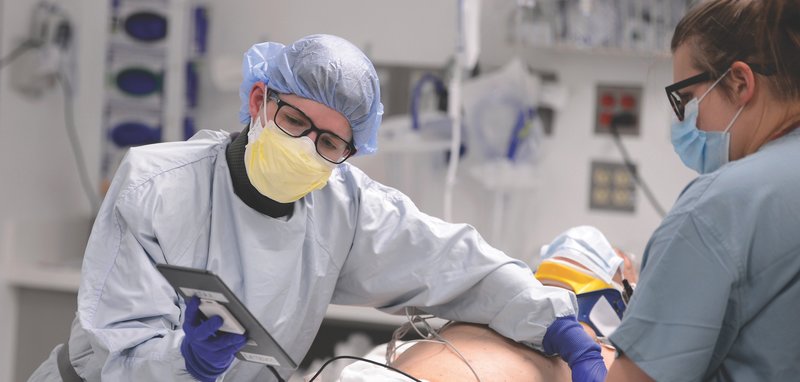
A student in the Special Operations Combat Medic Course uses a portable unltrsound while working alongside a trauma specialist from Cooper University Hospital in Camden, New Jersey. Army photo by Ken Kassens.
Encouraged by Chovanes, Kelly went to medical school and then returned to Camden for his surgical fellowship, and followed Chovanes into the Army Reserves in 2006.
Returning from Kandahar 10 years later, Kelly jumped in to help when he heard Chovanes wanted to bring SOCM students to Trenton.
But he had doubts about whether Trenont was a good fit.
“I was initially concerned that because we don’t have the volume that Cooper does, that the guys wouldn’t get as good of an experience,” Kelly said.

A student in the Special Operations Combat Medic Course, assesses a patient injured at a worksite in Trenton, New Jersey. Army photo by Ken Kassens.
But while Cooper is a teaching hospital associated with a medical school, Capital Health in Trenton is not. As a result, SOCM students get more time to work directly with trauma surgeons and staff.
One student there told The Forward Observer that a shift in Trenton was their favorite rotation. After a patient arrived late at night with severe head trauma, he’d been able to scrub into their emergency brain surgery, even performing minor skills under the surgeon's eye.
And doubts about Trenton as a training site evaporated four months after the program launched. In June of 2018, a local music festival erupted in gunfire between rival gangs, and 22 people were shot.
“They brought 17 of the 22 to us within about 25 minutes,” Kelly said. “People were literally at the scene just grabbing people that were shot and putting them in their cars and driving them to the hospital. One of the 18-Delta students grabbed the bag full of tourniquets and he was out front of the ER pulling people out of cars, putting tourniquets on, throwing them on stretchers.”
The next morning, New Jersey Gov. Phil Murphy visited the hospital. Kelly made sure he met the military students.
“I told Murphy, ‘I’m an Army surgeon in the Reserves with deployment experience in Afghanistan. We train these guys here in Trenton because the gun violence is so bad in this city that they get really good experience before they go to Afghanistan,’” Kelly said. “I don’t think the governor really liked to hear that, but it needed to be said."
This article first appeared in the Summer 2022 print edition of The Forward Observer, a special publication from Coffee or Die Magazine, as “Real-World Training.”
Read Next: Ukraine-Born Green Beret Raises Money to Send Supplies to War-Torn Homeland

Matt White is a former senior editor for Coffee or Die Magazine. He was a pararescueman in the Air Force and the Alaska Air National Guard for eight years and has more than a decade of experience in daily and magazine journalism.
BRCC and Bad Moon Print Press team up for an exclusive, limited-edition T-shirt design!
BRCC partners with Team Room Design for an exclusive T-shirt release!
Thirty Seconds Out has partnered with BRCC for an exclusive shirt design invoking the God of Winter.
Lucas O'Hara of Grizzly Forge has teamed up with BRCC for a badass, exclusive Shirt Club T-shirt design featuring his most popular knife and tiomahawk.
Coffee or Die sits down with one of the graphic designers behind Black Rifle Coffee's signature look and vibe.
Biden will award the Medal of Honor to a Vietnam War Army helicopter pilot who risked his life to save a reconnaissance team from almost certain death.
Ever wonder how much Jack Mandaville would f*ck sh*t up if he went back in time? The American Revolution didn't even see him coming.
A nearly 200-year-old West Point time capsule that at first appeared to yield little more than dust contains hidden treasure, the US Military Academy said.












