Scars Are Not Forever: How Operation Mend Helped Make a Marine Whole Again

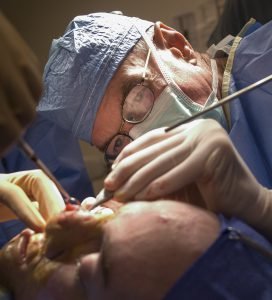
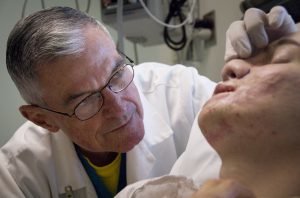
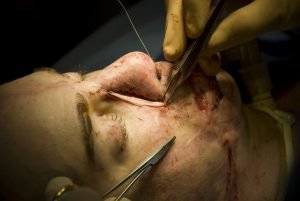
Dr. Timothy Miller, chief of reconstructive and plastic surgery at the University of California Los Angeles Medical Center, operates on Aaron Mankin’s nose Nov. 18 at UCLA Medical Center. Miller has operated on Mankin 12 times, and Mankin was the first wounded service member to take advantage of Operation Mend, a partnership between the U.S. military and UCLA Medical Center, through which UCLA provides world-class plastic reconstructive surgeries to disfigured service members. (Official U.S. Marine Corps photo by Staff Sgt. Ethan E. Rocke)
“Scars are not forever” was conceived for one Marine in the months of rehabilitation that followed an IED blast in Iraq, which left him badly burned and disfigured. Since then, the spirit of that ideal has evolved into an innovative partnership between military and civilian medicine that is actualizing, for some, that once rhetorical question: What if?
Aaron Mankin lay still on an operating table, bright halogen bulbs spilling light over every bit of his fire-scarred face: closed eyes placid with unconsciousness, relaxed jaw peeking out from the fissure between rich, disfigured lip tissue, an incision on the right side of his nose stretching the length of it.
The ordered bustle of the operating room lay outside, far above the anesthesia.
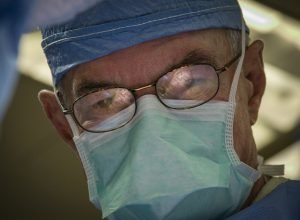
There, Dr. Timothy Miller, chief of reconstructive and plastic surgery at the University of California, Los Angeles Medical Center, looks down at Mankin’s face and focuses.
Coolly marking Mankin’s face with a pen earlier, Miller had described the goals of the procedure, Mankin acknowledging with a characteristic smile and nod – a gesture of enduring trust in the man whose scalpel has been to Mankin’s face what da Vinci’s brush was to his Mona Lisa.
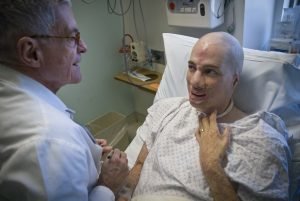
“I take your pictures home with me, ya’ know?” Miller said during the examination, referring to the dozens of photos he uses to track and plot the evolution of Mankin’s face before and after operating on it a dozen times.
Mankin reached to his throat to close the airway of his tracheostomy and push the air from his lungs up through his damaged vocal chords.
“Oh yeah?” he said, his soft, raspy voice contrasting smiling, wide eyes.
“Oh yeah,” Miller said, looking to Mankin’s mother, Diana Phelps, and nodding with a smile. “I do, really.”
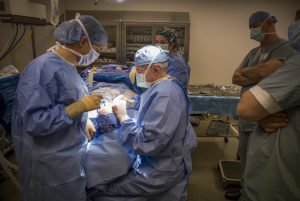
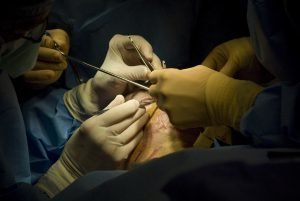
This is Mankin’s twelfth surgery under Miller’s hands – “magic hands,” say some of his coworkers and patients. The lofty, soothing melody of Frank Sinatra’s “Fly Me to the Moon” wafts in the operating room as Miller makes a precise and gentle sawing motion with his tiny scalpel, a handful of doctors and nurses looking on. He trims away unnecessary flesh from beneath Mankin’s nose – the nose he built with cranial bone and skin from Mankin’s forehead.
That was the first step. Now Miller needs to thin it out, make it better resemble Mankin’s old nose, the one he had before an explosion in Iraq left him badly burned about his arms and face – the nose from the pictures of the handsome, slender Arkansas boy with that coy twinkle of charisma. Miller takes to the task with the enthusiasm of an inspired artist.
“(These service members) have given a tremendous amount of their lives to me and my family,” Miller says. “If I can give something back to them, it’s very gratifying.”
The thin, boyish features Mankin inherited were supplanted May 11, 2005. Then Lance Cpl. Mankin was a Marine combat correspondent assigned to cover Operation Matador, a roughly weeklong mission to root out insurgents near the Syrian border north of the Euphrates River. Mankin was riding in an amphibious assault vehicle when a massive explosion from a roadside bomb rocked the 26-ton vehicle.
The violent blast threw Mankin down inside the vehicle. When the instant haze of chaos and concussion cleared, Mankin opened his eyes. He was on fire.
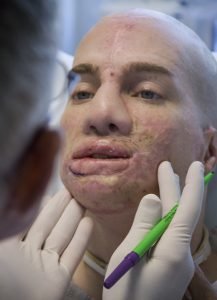
“The instinctive reaction at that point is to just gasp,” recalls the 26-year-old father of two. “That’s how I sustained most of my trachea injuries. I saw light at the back of the vehicle and just dove toward this dry, crusted earth. I rolled trying to get the fire out but couldn’t do it. I was exhausted, and I just closed my eyes and was ready to die. That’s when I heard the shouts of my fellow Marines saying ‘Put him out! Put him out!’”
The incident left Mankin with 25 percent of his body burned. His genetic predisposition to generate unusually high amounts of scar tissue caused his facial features to gradually contort, eventually twisting and fusing his nose and mouth area so much that his mouth shrank to a tiny, taut opening about an inch below an asymmetrical half-nose that, without its natural tip, displayed irregularly large nostrils and an upturned look.
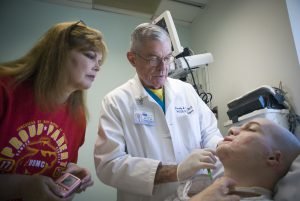
“Initially, Aaron’s face looked normal,” says his mother. “There were no visible wounds. And then it began to draw in and tighten up. I had to use a small funnel to feed him.”
Phelps helped care for her son for the first eight months he was a patient at Brooke Army Medical Center at Fort Sam Houston, Texas, where all of the U.S. military’s burn victims go for treatment. “BAM-C,” to which it is often affectionately referred, is one of the nation’s premiere trauma centers for burn victims, both military and civilian.
The hospital has cared for more than 4,043 service members wounded in the War on Terror, and the Army Burn Center there has treated 731 of those, according to hospital officials.
Mankin underwent about 40 surgeries at BAMC, including myriad skin grafts and an operation to open his mouth back up so he could eat normally.
But, according to Phelps, the limits of the medical center’s capabilities became apparent when the care required became a matter of aesthetics rather than physical rehabilitation.
“The doctors at Brooke are fantastic, but their focus is on function, not aesthetics,” she says.
President George W. Bush expanded the Defense Department’s healthcare funding by more than 200 percent since 2001, and the military made many advances in military medicine and healthcare infrastructure since the War on Terror began. But until recently, the military could not provide extensive reconstructive surgeries to its members.
General James F. Amos, assistant commandant of the Marine Corps, is among senior leadership at the Pentagon that has been at the forefront of the military’s recent efforts to address the shortfall.
“We’ve made great gains in recent years in expanding our continuity of care for wounded warriors, but change comes slow,” Amos says.
But in October 2007, the military’s slow, steady trend in healthcare advancement got sent into overdrive in the field of reconstructive surgery. The catalyst was an injection into the system from outside the government.
The prospect was revolutionary: One of the nation’s top hospitals offering up the services of its world-class, plastic reconstructive surgeons – no charge. It was exactly what the military needed to quickly bridge the gap between function and aesthetics for its disfigured warriors.
The man carrying the torch to the military was philanthropist Ronald A. Katz, a successful inventor and UCLA Medical Center board member.
“The concept was simple,” Katz says. “Why couldn’t we provide to these wounded service members not only the best medical care the military had to offer but the best the country could offer?”
Military leadership at BAMC and the Pentagon agreed, and a partnership was forged between the military and UCLA Medical Center, which U.S. News & World Report ranks as one of the top three hospitals in the nation and the top hospital in the western U.S. The partnership has since become known as Operation Mend.
In October 2007, Mankin became Operation Mend’s first patient. He was also, in large part, the inspiration for the program, according to Katz.
Katz and his wife, Madelyn, became involved with BAMC in 2006 when fundraiser and avid proponent of military and veterans’ causes Bill White invited the Katzes to San Antonio. Katz donated the lead gift at that time to a privately-funded project that brought to Fort Sam Houston in January 2007 two new Fisher Houses, which house families of wounded service members receiving treatment at BAMC.
“My wife and I visited the burn ward at Brooke, and we were particularly distressed by the number of facially disfigured service members,” Katz says.
A pivotal moment in Operation Mend’s conception occurred when Katz and his wife watched Mankin, whose charismatic personality and affinity for public speaking has attracted media attention and thrust Mankin into the limelight, on CNN in an interview with Lou Dobbs in November 2006.
“Lou asked Aaron, ‘What’s next for you?’” says Katz. “And Aaron said, ‘They’ve gotta’ fix the beautiful part … get me back to good looking.’ That really struck us.”
Katz says Mankin’s image and words that day were the beginning, but a final call to action came when the Katzes attended in January 2007 the opening ceremony for the Center for the Intrepid, a state-of-the-art physical rehabilitation center for amputees and burn victims adjacent to BAMC, and the new Fisher Houses, which Katz’s donations helped build. There were many disfigured service members at the ceremony.
“Seeing Aaron planted the seed, but seeing how many Aarons there are was the key,” Katz says. “At that point, we decided we should connect military commanders and my connections at UCLA.”
Katz says it took about six months to marry up the bureaucracies of BAMC and UCLA, and as the details of the partnership were worked out, Katz’s resolve and passion for the program became infectious within UCLA’s medical community.
“Once the program was announced, the byproduct was a wellspring of enthusiasm from people within the hospital to do something extraordinary for these service members,” he says. “The program is really two parts: medical care and personal care.”
Katz donated the first $1 million to fund Operation Mend and helped raise more than $10 million more. The private funds cover the costs of the surgeries as well as travel expenses for patients and their families, lodging, a living allowance and any extra medical expenses. The military’s health insurance provider, Tricare, covers the cost of hospitalization for patients.
“Although it’s expensive at our end, it’s a blessing to be able to use these funds to make such a difference in the lives of these soldiers and Marines,” Katz says.
Volunteers within UCLA’s medical community also provide patients with what Katz calls “buddy families.” Katz’s son Todd, his wife Dana and their children are the premier buddy family, providing friendship and support to Mankin, his wife Diana and their children during Mankin’s 12 trips to UCLA. Dana also oversees and coordinates the buddy family program.
“Everyone is compelled by the cause,” Dana says. “The CEO of UCLA Medical Center, called us and said, ‘Can we be a buddy family?’ When the CEO wants to be a buddy family, that’s not your typical bureaucracy.”
UCLA nurse Priscilla “Patti” Taylor, a retired Army nurse, also leads a community group of military veterans who sew “quilts of valor” for incoming patients.
Army Vice Chief of Staff Gen. Peter W. Chiarelli and Gen. Amos, the Corps’ second in command, have both visited Katz and other UCLA officials in recent months to talk about expanding Operation Mend.
“Programs like Operation Mend have shown us that sometimes the private sector can inject a capability into the system that we don’t have,” Amos says.
Katz says it is his hope that Operation Mend will expand beyond plastic reconstructive surgery.
“Fortunately, UCLA has extraordinary talents in many areas,” he says. “Our hope is that we will involve ourselves with other DoD hospitals that care for patients other than burn victims. If they need certain expertise that we can provide, we think UCLA has a lot to offer.”
In the meantime, Katz says Operation Mend currently has the funding and resources to continue providing reconstructive surgeries to any service members who need them, and he hopes to see other hospitals follow UCLA’s lead.
“We’re not the only place in the world that has extraordinary capabilities and talents,” he says. “I think in the next year or so, there is a possibility that this could expand to other medical centers of excellence, and if they need guidance, we can transport that to them.”
Amos says if other hospitals in the private sector are willing to further expand the care the military can provide, “We are more than ready to embrace that willingness and build a partnership.
“The Marine Corps and the DoD are fully committed to providing world-class care to our wounded warriors, but there is always room for improvement, and there may, in certain areas, be limitations to what military medicine can provide.”

Operation Mend has provided 43 surgeries to seven soldiers and Marines since October 2007, and 10 more patients are currently scheduled to undergo surgery in 2009, according to UCLA officials.
Mankin and his mother tried to express what those numbers mean to the people whose lives they affect.
“Early on in my recovery I adopted the notion that ‘scars are not forever’ as a mindset,” Mankin says. “It was an articulation of my acceptance that this is the way I’m going to look for the rest of my life, and, with that, I’m not going to let my physical appearance keep me from being who I am and reaching the goals I set for myself.
“That mindset evolved when individuals from the other side of the nation opened up their hearts and their homes and said to me, ‘This is a reality we can give to you.’ And for them to seek me out and ask, ‘Can we do this for you?’ is an overwhelming blessing and I think speaks to the true spirit of the American people.”
Choking up, Phelps echoed her son’s sentiment, “There’s not a deep enough place inside me that could explain the gratitude for what they’ve given and what they’ve done and what they’re doing, not just for Aaron, but for everyone. There’s not a deep enough place.”
This article was originally published in Marines Magazine in 2008. Operation Mend and the services it provides has since grown significantly and continues to provide advanced surgical and medical treatment for post-9/11-era warriors injured during combat operations or while training for service, as well as comprehensive psychological healthcare and social support for both wounded warriors and their family members.

Ethan E. Rocke is a contributor and former senior editor for Coffee or Die Magazine, a New York Times bestselling author, and award-winning photographer and filmmaker. He is a veteran of the US Army and Marine Corps. His work has been published in Maxim Magazine, American Legion Magazine, and many others. He is co-author of The Last Punisher: A SEAL Team THREE Sniper’s True Account of the Battle of Ramadi.
BRCC and Bad Moon Print Press team up for an exclusive, limited-edition T-shirt design!
BRCC partners with Team Room Design for an exclusive T-shirt release!
Thirty Seconds Out has partnered with BRCC for an exclusive shirt design invoking the God of Winter.
Lucas O'Hara of Grizzly Forge has teamed up with BRCC for a badass, exclusive Shirt Club T-shirt design featuring his most popular knife and tiomahawk.
Coffee or Die sits down with one of the graphic designers behind Black Rifle Coffee's signature look and vibe.
Biden will award the Medal of Honor to a Vietnam War Army helicopter pilot who risked his life to save a reconnaissance team from almost certain death.
Ever wonder how much Jack Mandaville would f*ck sh*t up if he went back in time? The American Revolution didn't even see him coming.
A nearly 200-year-old West Point time capsule that at first appeared to yield little more than dust contains hidden treasure, the US Military Academy said.












